Last year, Dr. Eva Feldman was named the James W. Albers Distinguished University Professor, the University of Michigan's highest faculty honor. Dr. Feldman chose to name hers after her longtime friend and mentor, Dr. James … [Read more...]
Mini Symposium Series: Environment, Health & Policy
In our latest installment, U.S. Rep. Debbie Dingell sat down to talk to Dr. Eva Feldman about the environment, health, and public policy. Afterward, Dr. Feldman was joined by two esteemed panelists, Drs. Bhramar Mukherjee and … [Read more...]
Michigan Medicine Health Lab Features Groundbreaking ALS Research
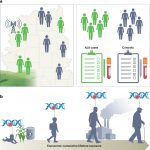
Health Lab: Drawing a tube of blood could assess ALS risk from environmental toxin exposure The risk score included 36 pollutants persistently found in the environment Author | Noah Fromson Jacob Dwyer, Justine Ross, … [Read more...]
Gut Microbiome Provides New Therapeutic Target for ALS
Brain, one of the top academic journals, published groundbreaking new research by Dr. Feldman et al. that looked at the connection between the microbiome, fatty acids in the blood, and ALS. In the gut microbiome are a … [Read more...]
The ALS Exposome in Nature Reviews Neurology
Just what is the exposome? Eva Feldman, M.D., Ph.D., James W. Albers Distinguished University Professor, and Russel N. DeJong Professor of Neurology, explains that it is the amalgamation of what comes into our body from … [Read more...]
MedSciWriters Features Dr. Feldman in Scientist Spotlight
For ALS Awareness Month (May), the University of Michigan student organization chose Eva Feldman, M.D., Ph.D., to appear in their "Scientist Spotlight" feature to talk about the … [Read more...]
Clinic Q&A: Nurse & Nerve Center Sandy Lemkin
The theme for Nurses Week this year is “You Make a Difference.” In our own Pranger ALS Clinic is a perfect example of someone who not only makes an incredible difference in the lives of so many ALS patients and their families but … [Read more...]
10 Key Facts About ALS in 2023
Last year, Dr. Eva Feldman published a seminal ALS seminar in the top academic journal The Lancet. In honor of ALS Awareness Month (May), she pulled out the ten key facts that are important to know in 2023. Some even surprise … [Read more...]
Clinic Q&A: The Power of Social Work with Darla Goulet
Few professions match the powerful impact of striving to empower and improve the lives of those around them the way social work can. There is a very special person who has been filling this crucial function for the past seven … [Read more...]
Journal Cover Features Latest ALS Research
A team led by Pranger ALS Clinic Director Stephen Goutman, M.D., M.S., and Director of both the ALS Center of Excellence and NeuroNetwork for Emerging Therapies Eva Feldman, M.D., Ph.D., recently published a study in the academic … [Read more...]
- 1
- 2
- 3
- …
- 11
- Next Page »